As both government and commercial payers direct a greater share of volume to out-patient facilities and patient demand for same-day service increases, opportunity and competition in the ambulatory surgical center (ASC) space are increasing. The U.S. ASC market size is projected to grow to more than $75 billion by 2030 and in January 2024, CMS announced the addition of 41 new billing codes for covered procedures for ASCs. More CMS billing codes means more claims data, and with price transparency data now available, ASCs have more leverage than ever to negotiate competitive contracts with payer partners. In order to capture this opportunity, managed care teams seek to differentiate themselves in the market through comprehensive price and performance insights. “For managed care leaders in ASCs to succeed in their role, all paths must start with data collection – only you understand your business best – not a consultant, not an advisor, not a vendor, and not the payer you’re negotiating with.” – Neechi Mosha, SVP of Growth, Clarify Health The good news is with ASCQR, OAS CAHPS, and now price transparency, CMS-certified ASCs are no strangers to data collection and analysis. The opportunity for managed care teams lies in linking price, quality, outcomes, and market data to communicate their unique value in contract negotiations with payers. Here are five ways managed care teams can use price transparency and performance data to strengthen their position in the market: How saturated is it? What rates are other ASCs being reimbursed for the same services and the same payers? What other ASC options are available around you? Is there an ASC in your market you should merge with or acquire? By analyzing reimbursement rates, market saturation, and potential merger/acquisition opportunities, ASCs can gain a competitive edge. For example, a managed care team can identify underserved areas within their market and strategically expand their network by acquiring or merging with existing ASCs. Precise insights into physician and facility performance and rate benchmarks are crucial for making informed investment decisions. What is the quality of care that your physicians are delivering in your ASCs? Leverage case mix-adjusted performance scores to talk to the CMO and their medical directors at health plans to share this information on how you benchmark against other ASCs and competitors. Utilizing case mix-adjusted performance scores, ASCs can effectively communicate the quality of care delivered by their physicians. This information can be shared with health plans to demonstrate how the ASC benchmarks against competitors and other ASCs regarding quality metrics. Compare your rates against those of competitors and apples-to-apples to show where you’re saving dollars for your health plan partners. By comparing rates against competitors and illustrating cost savings, ASCs can demonstrate the financial benefits of partnering with them, which are not always readily apparent. See what procedures and services are being delivered by site of care in your market or markets you’re expanding to and assess what additional savings you can drive by shifting more of that volume. Analyzing procedures and services delivered by site of care allows ASCs to identify opportunities for driving more volume. By shifting procedures from higher-cost settings to ASCs, additional savings can be achieved. For instance, if data shows that certain procedures can be performed cost-effectively in an ASC setting, managed care teams can negotiate for increased volume allocation. Are there creative ways to frame your asks based on this data? An example of this in practice would be negotiating an increased Medicare rate given the savings realized from shifting spend out of a hospital setting. Data-driven insights enable ASCs to identify creative negotiation strategies. For example, by providing data on cost savings achieved by shifting procedures from hospital settings to ASCs, managed care teams can negotiate for higher reimbursement rates or other favorable terms. Data collection is key for ambulatory surgery centers looking to differentiate themselves in the market. By gathering comprehensive price and performance insights, ASCs can better understand their strengths, weaknesses, and opportunities for improvement. This data-driven approach allows managed care leaders to make informed decisions that can lead to better negotiation outcomes with payers and ultimately improve the overall efficiency and quality of care provided. Rather than relying solely on external sources like consultants or vendors, ASCs have the unique advantage of understanding their own business intricately. This internal knowledge, coupled with robust rates data collection and analysis, empowers ASCs to tailor their strategies and operations to meet the specific needs of their patients and the demands of the market. With growing opportunity and competition, ASCs that prioritize data-driven decision-making are better positioned to thrive and deliver exceptional value to their patients and stakeholders.1. Understand your market
2. Communicate your quality of care
3. Explain your savings
4. Show the impact of driving more volume
5. Find opportunity
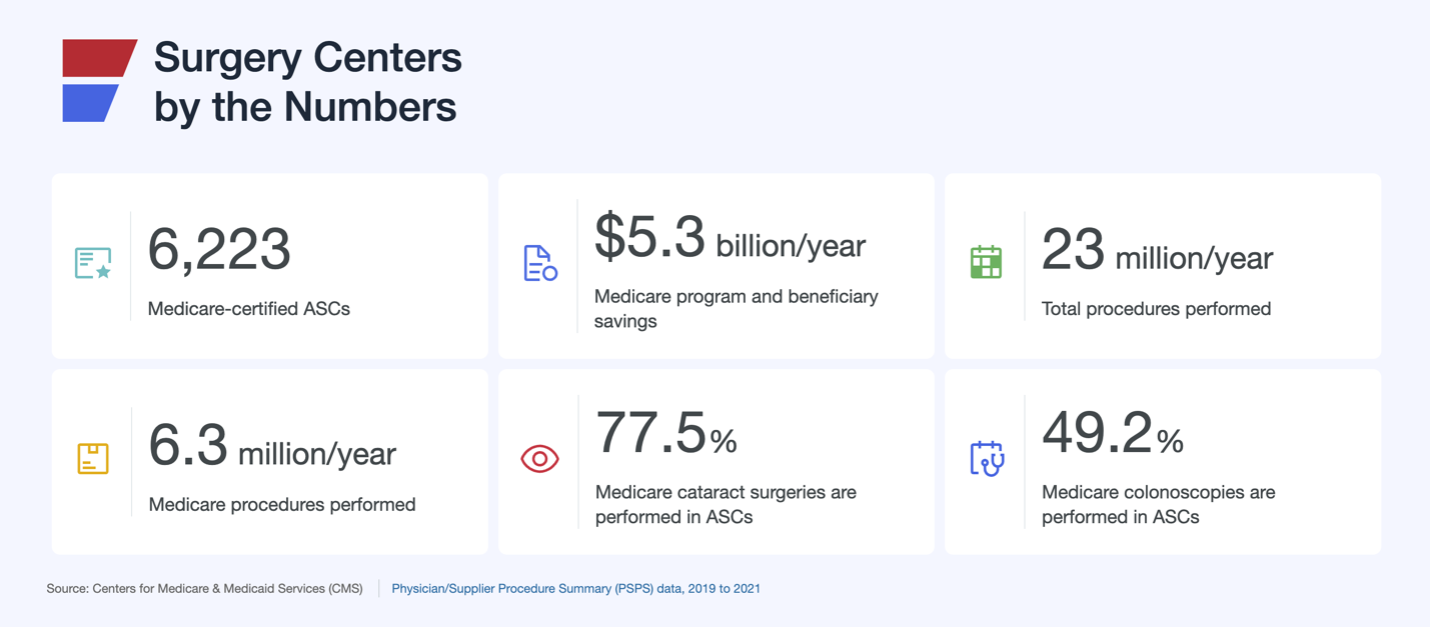
ASC performance and price transparency data
- Author Details