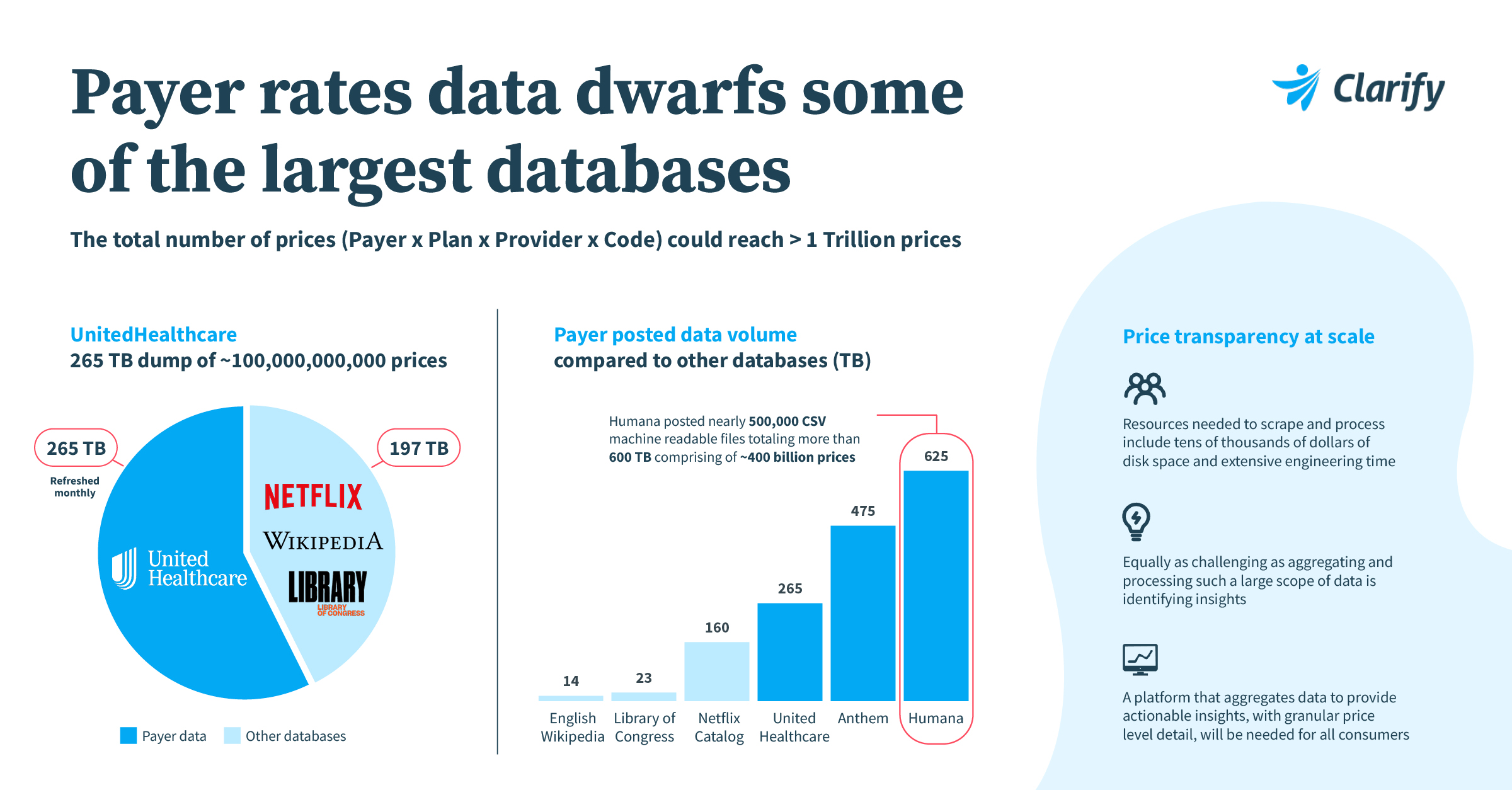
Over the last 20 months, the healthcare industry has been working toward compliance with the Centers for Medicare & Medicaid Services (CMS) Hospital Price Transparency and Health Plan Transparency in Coverage mandates, which require healthcare providers and health plans to post pricing information for covered items and healthcare services online. However, many leading organizations are pushing beyond compliance to capture the true value of these rulings and the data they create for research, business analytics, and the realization of the Triple Aim. Stakeholders across healthcare need access to democratized price transparency data to move away from dated incentive and contracting models – those that encourage the nondisclosure of pricing data. Creating greater price transparency helps move the market to a fairer median for all stakeholders in the healthcare ecosystem. Doing this essentially puts dollars back in the pockets of patients who bear the brunt of having to pay continuously higher premiums as healthcare costs rise year over year. At Clarify, transparency is at the heart of everything that we do. You’ll find no black boxes here. We are actively processing and integrating healthcare pricing and rate data into more and more of our solutions to ensure we’re empowering the market and our customers to create better, more competitive services and engage in more transparent payment arrangements with one another. One of the early things we discovered in bringing in provider rates data is that there were significant inconsistencies in file formats that the hospitals were posting on their websites, as well as in the information included in their files. This variation in files made public by hospitals is likely an indication of the technical prowess of those organizations and the level of resources required to deliver the appropriate machine-readable file formats. Despite being messy, those rates files were small enough that any health plan or provider group interested in a hospital could easily have gone to its website, pulled down its rates file, and opened it up within Excel. Since July, with payer-posted rates data becoming available, the scenario has evolved considerably. These rates have, up to this point, been discussed in negotiation rooms and never been made available to competitors, much less to consumers, which is why a person can go for a lab test that may cost $40 at place A and pay $400 for that same test across the street at place B. There’s a huge appetite in the market to have access to greater price transparency that will start unlocking opportunities to normalize prices across the market. We’ve also observed that payer rate data is more standardized than hospital-published data. Payers are demonstrating a high level of compliance with what needs to be included in those files. However, compared to hospital data which is more manageable in size, this payer-published data is extremely cumbersome and challenging to normalize and aggregate. Why? Well, if you were to think of one hospital system’s rates data versus one month of payer rates files, you’re looking at file sizes seven million times larger, if not more. On top of that, the payer data is refreshed monthly. United Healthcare’s price transparency website contains over 56,000 files in a JSON format that add up to roughly 100 billion prices if you were to pull all those files together, normalize them, and look at all the prices across varying procedures and contract negotiations. Similarly, Humana posted roughly 600 terabytes of data. This is significantly larger than Netflix’s entire movie library, the Library of Congress, and the English Wikipedia. The volume of data that’s being made available through these price transparency mandates is on a scale that is hard to really wrap our minds around. Payer rates data dwarfs some of the largest databases including Netflix, the Library of Congress, and the English Wikipedia. How is Clarify positioned to best help the healthcare ecosystem leverage rates data? Having made considerable investments to build the industry’s most powerful data ‘refinery’ to normalize and optimize massive amounts of data and convert them into actionable insights, Clarify is in a unique position to wrangle all of this provider and payer data. Playing our part in creating the level of price transparency the healthcare industry deserves is integral to our mission to power better care. We believe that the combination of rates data with Clarify’s trusted provider performance benchmarks will help more precisely determine where patients should go for higher-quality care at a more affordable cost. Additionally, provider organizations are leveraging rates insights together with performance measures, market intelligence, and patient journey insights to optimize patient journeys, increase patient loyalty, build stronger affiliations, and make better investment decisions. With Clarify, health plans can seamlessly leverage rate intelligence data combined with provider performance insights to build higher-performing networks and stronger value-based contracts with their provider partners. Our solutions bring transparency and trust that the industry has previously never had access to.
- Author Details





