
CLARIFY MERIDIAN
Great Health Systems
Don't Just Deliver Care.
They Orchestrate It.
The care that's best for patients is also the care that makes the system sustainable. Clarify Meridian is how health systems prove it.
Meridian unifies referral intelligence, physician activation, consumer engagement, and outcomes attribution into a single platform. It is the product of years of partnership with health systems, built on the most complete picture of care economics in healthcare, and delivered by a company whose outcomes are tied to yours.
NEWS AND ANNOUNCEMENTS
Clarify Health Names Co-Founder Todd Gottula CEO, Unveils New Leadership Team
THE CHALLENGE
A Trillion-Dollar Blind Spot.
Every day, health systems make thousands of referral decisions that direct over $1 trillion in annual U.S. healthcare spending, with almost no unified data to guide them.
The numbers tell the story. Thirty to fifty percent of specialty referrals are never completed. At large systems, 40–60% of referrals leak out-of-network. Median operating margin has compressed to 1.5%, while the average large health system now operates across 70+ payment frameworks simultaneously.
Most organizations sense the opportunity. They can't see it clearly enough to act. And no existing technology has been built to optimize across all of it.
Meridian sees what’s being left on the table and helps you capture it.
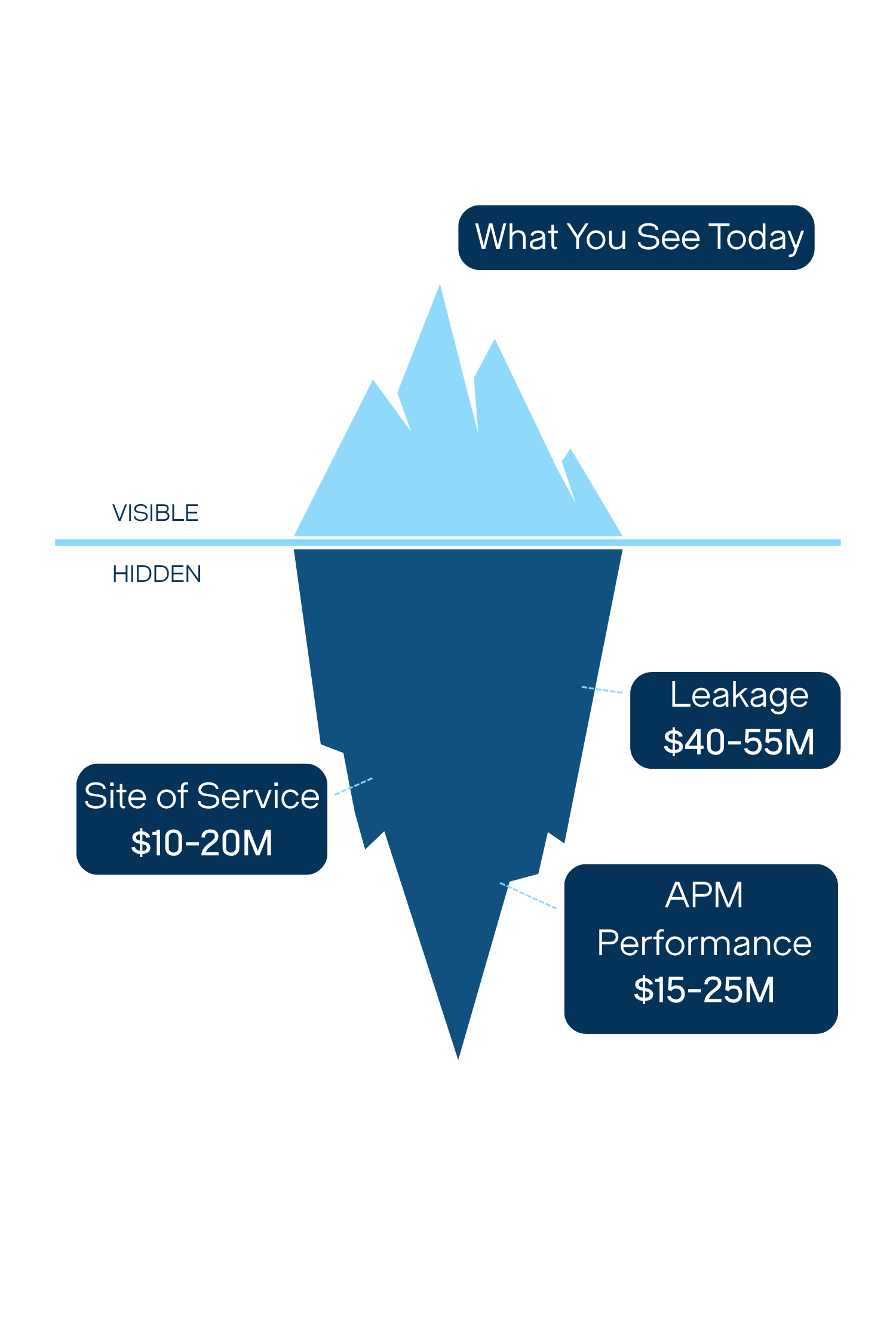
For a typical large health system, the gap between current performance and full potential represents $65–$100 million in annual opportunity left on the table, year after year.
THE SOLUTION
Introducing Clarify Meridian.

Clarify Meridian answers the questions no other system can: which referrals to optimize, which specialists deliver the best outcomes for each contract, and what the financial impact looks like before any action is taken.
It is the first platform to unify referral intelligence, physician activation, consumer engagement, and outcomes attribution, transforming referral management from reactive tracking to proactive orchestration.
The result is a health system that reduces leakage, strengthens referral performance, and captures more value from its network. Systematically. Repeatably. At scale.


60K+
Cases lost to leakage
per health system annually
$65–100M
Annual opportunity per health system
$3.2B
Documented customer ROI
70+
Payment models across FFS and VBC
THE DELIVERY MODEL
A New Model. Aligned Incentives.
Clarify delivers Meridian as a tech-enabled outcomes partnership, deploying both the platform and dedicated Success Services teams directly into health system operations, with economics tied to measurable results.
That means when your margins improve, when keepage is recaptured, when the network compounds — that's when we succeed. Not before.
This is what it means to be an outcomes company.
CLARIFY ATLAS PLATFORM®The Data Foundation That Powers Meridian
Meridian runs on the Clarify Atlas Platform — a decade-built data foundation that gives health systems a view of their network no other platform can provide.
300M+
Patient Lives
Longitudinal patient records spanning every care setting — primary, specialty, post-acute, and behavioral health — across the full U.S. population
5.6T
Price Transparency Rates
Actual negotiated rates from every payer-provider contract — not blended estimates, not market averages. The most granular commercially available rate dataset in healthcare
70+
Payment Models
Every major VBC arrangement — shared savings, bundles, capitation, P4P, episodic — modeled simultaneously for every referral decision
20B+
AI Predictions
Machine learning models trained on a decade of outcome and cost data — powering quality predictions, cost estimates, and care pathway recommendations at the patient level
Ready to transform
your referral network?
Schedule a personalized briefing with our team. We'll show you the opportunity value specific to your organization — and how you can capture it.
